Access & Closure, Acute Kidney Injury (AKI), Clinical Research & Data, AMI Cardiogenic Shock
Katherine Kunkel: Troubleshooting with an Eye on the Prize
“How can we leverage what we learned from DanGer Shock,” asks Katherine Kunkel, MD, MSEd, FACC, FSCAI, “to further improve our outcomes in our patients and reduce our adverse events?”
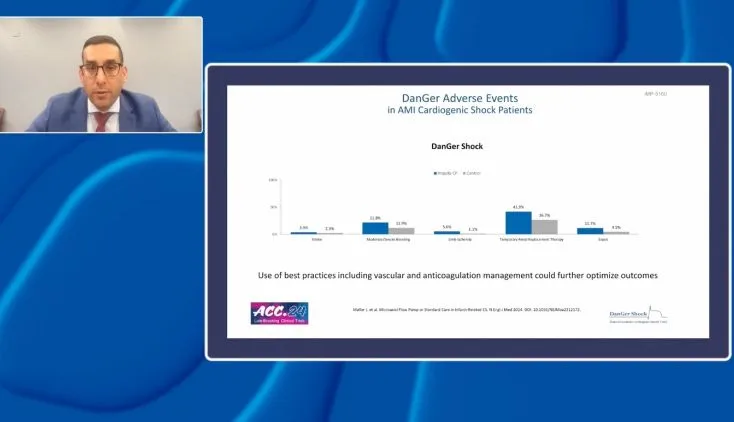
Dr. Kunkel, an interventional cardiologist at Piedmont Heart Institute in Atlanta, Georgia, highlights the key findings from the DanGer Shock RCT: Routine use of Impella reduces all-cause mortality at 180 days in AMI cardiogenic shock due to STEMI compared to standard care alone with an absolute 12.7% reduction in mortality with a number needed to treat (NNT) of 8 patients to save 1 life. She then focuses on the vascular complications (moderate/severe bleeding and limb ischemia) and need for temporary renal replacement therapy seen in the study.
With regard to vascular complications, Dr. Kunkel emphasizes, “we have more control in the cath lab than at any other time for this complication.” With this in mind, she highlights the following best practices for minimizing vascular complications.
- Use a combination of ultrasound and fluoroscopy for access 100% of the time in preparation for adeptly handling emergencies.
- Use micropuncture access with an angiogram to know where you are.
- Plan for closure at the time of device insertion, preferably with a Perclose device if feasible.
- Assess distal limb perfusion immediately before leaving the cath lab and serially in the ICU, placing a distal limb perfusion catheter if needed.
Dr. Kunkel reviews ultrasound access techniques as well as Perclose and Manta closure techniques. She emphasizes, “The best closure is a safe closure” and explains that surgical repair should be considered if safe closure cannot be obtained percutaneously.
With regard to temporary renal replacement therapy, Dr. Kunkel explains that it is important to acknowledge survivorship bias in the DanGer Shock trial. “When you think about outcomes that clinically matter to your patients,” she states, “keep in mind, only 3 patients in the trial, or 1.7%, remained on dialysis at 90 days. And so, short-term, inpatient renal replacement therapy may not be the worst thing, again, with a life-saving therapy.”
To mitigate the risk of patients requiring temporary renal replacement therapy, Dr. Kunkel highlights the following best practices:
- Get an admission echocardiogram for placement when the patient arrives in the ICU.
- Monitor for hemolysis by regularly checking urine and labs.
- Ensure adequate preload and monitor afterload.
- Address all alarms on the device.
- Ensure adequate anticoagulation.
“It’s important to have a savvy team,” she emphasizes, “who can understand and address all alarms on the Impella device whether it’s 2 o’clock in the afternoon or 2 o'clock in the morning.”
“These are tremendously sick patients,” Dr. Kunkel concludes, reiterating that DanGer Shock demonstrates that clinicians can save 1 in every 8 patients who would not have survived on standard of care. “And I think that is worth fighting for, and that is worth continually working on improving and getting better in the way that we care for our patients.”
NPS-5088